Better Night
BestsellerUnwind & wake up refreshed with Better Night
Better Night is a supplement formulated to support relaxation and night time balance as part of your evening routine.
During perimenopa...Read More
Better Night is a supplement formulated to support relaxation and night time balance as part of your evening routine.
During perimenopause and menopause, natural hormonal changes may make it harder to unwind and switch off at night.
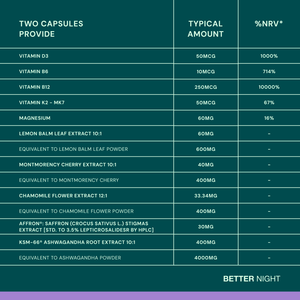
Developed by doctors, Better Night combines selected botanicals, vitamins and minerals, including Ashwagandha KSM-66®, Affron® saffron, magnesium glycinate and vitamins B6, B12 and D3, to support relaxation and normal nervous system function.
Read Less- Tiredness & fatigue
- Nervous system support
- Healthy sleep patterns
- Relaxation support
- Free UK shipping
- Flexible delivery options
- Pause, skip, or cancel anytime
- Earn 3% store credit
- Free UK shipping
- Flexible delivery options
- Pause, skip, or cancel anytime
- Earn 3% store credit
Store pickup unavailable

5 / 5
5 / 5
"I would decribe Better Night as 'brilliant' it's so helpful and it genuinely works, it's amazing the difference taking 2 little capsules at night can make."
How Better Night works to support you nightly
Why sleep disruption is so common in perimenopause
Why sleep disruption is so common in perimenopause
During perimenopause, levels of progesterone, the hormone that plays an important role in promoting calm, begins to decline. Progesterone helps the body feel more settled and resilient to stress, so as levels fall, many women find they feel less able to cope with everyday pressures.
At the same time, hormonal fluctuations can make the nervous system more reactive. This can show up as heightened anxiety, a racing mind, or waking during the night with sudden, intrusive thoughts, even when nothing in particular feels “wrong”.
It’s also why sleep can feel lighter or more fragmented, and why early-morning waking becomes more common during this stage. These changes are common, but they can feel unsettling when they appear suddenly.
How Better Night's expert blend supports your sleep
How Better Night's expert blend supports your sleep
Better Night brings together a carefully balanced blend of botanicals, vitamins and minerals, chosen to support relaxation, emotional balance and night-time recovery when sleep feels harder to come by.
At the heart of the formula are trademarked, clinically studied forms of ashwagandha (KSM-66®) and saffron (Affron®). These ingredients have been selected for their role in supporting the body’s response to stress and emotional wellbeing, helping the mind feel calmer as you move towards sleep.
Supporting botanicals including lemon balm and chamomile are included for their traditional use in relaxation and winding down in the evening, while Montmorency cherry provides a natural source of compounds associated with the body’s natural sleep-wake rhythm.
To complete the blend, magnesium glycinate and vitamins B6, B12 and D3 support normal nervous system and psychological function. Vitamin K2 is included alongside vitamin D3 to support optimal absorption, ensuring these nutrients can be used effectively by the body.
Each ingredient has been selected not just for its individual role, but for how it works together as part of a gentle, non-sedating formula designed to support better rest, night after night.
Simple to take, easy to fit into your routine
Simple to take, easy to fit into your routine
Better Night is designed to be taken in the evening as part of your wind-down routine.
Our recommended dose to support mood and sleep is:
- 2 capsules in the evening
- Around 1 hour before bed is optimal
For longer-term use, a lower dose of 1 capsule each evening can also be taken, depending on your individual needs.
Taking Better Night helps support relaxation and night-time recovery, allowing the carefully balanced blend to work gently overnight.
Flexible subscriptions for consistent, reliable support
Flexible subscriptions for consistent, reliable support
Better Night is designed to be taken consistently, which is why we offer flexible subscription options to support your routine over time.
You can choose:
- Monthly delivery, or
- 3-month delivery, depending on what suits you best
Subscriptions help ensure you never run out, while giving you full control at our best price.
You can pause, skip or cancel at any time, directly from your account.
Because Better Night contains ashwagandha, some women choose to cycle their use, taking a short break after around six months of continuous use. This is a personal choice and not a requirement. Our subscription model makes this easy, allowing you to pause and restart whenever it feels right for you.
Think of Better Night as supportive, flexible care that adapts to your needs, rather than a fixed routine.
Developed by women’s health experts who’ve been there too


"Better nights make for for better days"
"If your sleep is suffering and your mood is low during perimenopause, Better Night's potent blend of high quality ingredients is a great addition to your menopause toolkit."
- Dr Shahzadi Harper, Women's Health Specialist and Resident Doctor at The Better Menopause
As seen & celebrated in the Press
Meet the women who are sleeping better with Better Night








Genevieve
Customer
"I've found Better Night so helpful, they are absolutely briliant, I've been taking an hour before bed and finding i'm getting off to sleep much easier and importantly, i'm staying asleep."
Andrea McClean
Customer
"I would decribe Better Night as 'brilliant' it's so helpful and it genuinely works, it's amazing the difference taking 2 little capsules at night can make."
Cherry Healey
Customer and advocate
"Without good sleep, I'm not nice to be around, Better Night has helped me get that good sleep!"
Rosie
Customer
"Honestly, since I've been taking Better Night my sleep has been so much better. I'm so grateful to The Better Menopause for formulation this product."




Debbie Wosskow, OBE
Founder
"I've never been a great sleeper, which is why we wanted to create a sleep supplement that works. I can honestly say taking Better Night has been transformational for my sleep."
Stephanie de Chillaz
Nutritional Therapist
"I absolutely love the high quality ingredients in Better Night, it works wonders for my sleep."
A targeted blend for ultimate mind and sleep support
Alongside vitamins B6, B12 and D3, each ingredient has been expertly selected for its role in supporting relaxation, recovery and night-time balance for women during perimenopause and menopause.
Ashwagandha KSM-66®
Ashwagandha KSM-66® is a highly researched, full-spectrum extract of ashwagandha root, selected for its quality, purity and clinical backing. It’s included to help support emotional balance and relaxation when stress or a racing mind make it harder to switch off at night.
Studies suggest it may help to:
- Support a calmer response to stress
- Promote relaxation and emotional balance
- Support better sleep quality over time

Affron® (Saffron)
Affron® is a patented saffron extract of the highest quality. It helps to support mood balance and a calmer mental state when emotional restlessness interferes with sleep.
Studies suggest it may help to:
- Support a positive mood
- Reduce feelings of emotional tension
- Promote a calmer mindset before bed

Magnesium glycinate
Magnesium glycinate is a highly absorbable form of magnesium that’s gentle on the digestive system. It’s included to support relaxation and help the body feel more settled at night.
Supports:
- Normal nervous system function
- Muscle relaxation
- Reduced tiredness and fatigue

Montmorency cherry
Montmorency Cherry is a natural source of melatonin, a hormone involved in regulating the body’s sleep–wake cycle. It’s included to support night-time balance and help reinforce healthy sleep patterns.
Naturally supports:
- The body’s natural melatonin levels
- A healthy sleep–wake rhythm
- More consistent night-time rest

Lemon balm leaf
Lemon balm is a traditional botanical known for its gentle, soothing properties. It’s included to support relaxation and help the body wind down naturally in the evening.
Traditionally used to help:
- Ease nervous restlessness
- Support relaxation in the evening
- Promote a calmer transition to sleep

Chamomile
Chamomile is a well-known botanical traditionally used to support relaxation and comfort. It helps support evening calm when the body feels tense or unsettled.
Traditionally used to help:
- Encourage relaxation
- Support evening comfort
- Promote restful sleep habits

Support for calmer evenings and more restorative sleep
-

Calms the mind and supports the nervous system
-

Supports quality sleep and overnight restoration
-

Non-habit forming and suitable for nightly use
-

Simple capsule form – no taste, no liquid, no powder
-

Calms the mind and supports the nervous system
-

Supports quality sleep and overnight restoration
-

Non-habit forming and suitable for nightly use
-

Simple capsule form – no taste, no liquid, no powder
What to expect on your Better Night journey

What to expect on your Better Night journey
Settle into your new evening routine, take 2 capsules in the evening, ideally around 1 hour before bed, as part of your wind-down routine. Consistency matters more than perfection, the aim is to help your body recognise it’s time to slow down.
Within 1–2 weeks, many women begin to notice a calmer mind in the evening, less restlessness, and an easier transition into sleep. Night-time waking may start to feel less disruptive as your body adjusts.
With continued use, sleep often feels deeper and more refreshing, with fewer disturbances such as night sweats or anxious waking. Keep going, the benefits tend to build as Better Night supports night-time recovery consistently.
Real results from women feeling the difference
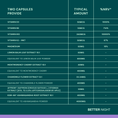
After two months of consistent evening use, participants in our impact study reported improvements in sleep quality and overall evening comfort.
saw a reduction in mid night wake-ups
saw a reduction in night sweats
reported a noticeable reduction in fatigue
Still have questions? we’re here for you
View our most common FAQs below or contact us by tapping below.
Will Better Night make me feel drowsy or groggy during the day?
Will Better Night make me feel drowsy or groggy during the day?
Better Night is designed to support relaxation in the evening, not to sedate. It does not contain sleep medications and is non-habit forming.
Some women who have been sleeping poorly for a long time may notice they feel more tired at first, as their body begins to recover from accumulated sleep debt. This usually improves as sleep becomes more settled and consistent over time.
When should I take Better Night?
When should I take Better Night?
We recommend taking 2 capsules in the evening, around 30 minutes to 1 hour before bed.
As your body becomes more rested, some women find that 1 capsule each evening is enough for ongoing support. It’s always best to listen to how your body responds over time.
Can I take Better Night alongside other Better Menopause supplements?
Can I take Better Night alongside other Better Menopause supplements?
Yes. Better Night has been designed to work alongside the rest of The Better Menopause range.
Many women choose to take it alongside Better Gut as part of our of a wider routine that supports overall wellbeing through perimenopause and beyond.
Better Night and Better can be purchased togter as part of our Serenity Bundle.
Is Better Night non-habit forming? Can I take it long term?
Is Better Night non-habit forming? Can I take it long term?
Yes. Better Night is non-habit forming and designed for regular use as part of an evening routine.
It supports the body’s natural ability to unwind rather than forcing sleep. Many women choose to take Better Night consistently over the longer term.
Because the formula contains ashwagandha, some women prefer to cycle their use, taking a short break after several months of continuous use. This is a personal choice rather than a requirement, and our flexible subscriptions make it easy to pause and restart whenever it feels right for you.
I’m taking HRT. Can I take Better Night as well?
I’m taking HRT. Can I take Better Night as well?
Yes, Better Night can be taken alongside hormone replacement therapy or prescribed hormone treatment.
I’ve had cancer treatment. Can I take Better Night?
I’ve had cancer treatment. Can I take Better Night?
The ingredients in Better Night do not have any known contraindications for women with a history of cancer.
However, if you are currently undergoing treatment or taking prescribed medications, we recommend speaking with your GP, oncologist or healthcare team before starting any new supplement.
I wake up in the night or very early in the morning. Is Better Night still suitable?
I wake up in the night or very early in the morning. Is Better Night still suitable?
Yes. Night waking and early-morning waking are common during perimenopause and beyond.
Better Night is designed to support relaxation and night-time recovery overall, which may help support more settled sleep patterns when taken consistently.
Does Better Night contain fillers or unnecessary additives?
Does Better Night contain fillers or unnecessary additives?
No. We’ve worked carefully to keep the formulation as clean as possible.
Only natural bulking and flow agents are used, including brown rice and bamboo extract.
Build on your Better Night foundation your way
- CSClaira S.Verified BuyerI recommend this productRated 5 out of 5 stars9 hours agoI was skeptical, however...
Exceptionally delighted!
This product is very good indeed. It's gentle on your tummy and I've really noticed a difference in my quality of sleep, which I will never take for granted! Sleep is one of the most important functions for a happy life. Therefore, I shall keep taking these, although quite expensive, I feel they are worth every penny. If you are struggling with your sleep pattern, do give these a go!
Was this helpful? - JTJennifer T.Verified BuyerI recommend this productRated 5 out of 5 stars1 week agoGreat product
fantastic i now get a better night sleep
Was this helpful? - JSJoanna S.Verified BuyerI recommend this productRated 5 out of 5 stars2 weeks agoeffective for me
i have found that taking this for a month has really helped my sleep - so have just reordered. I hope the effect is sustained, as it has been lovely to have great sleep again!
Was this helpful? - MSMrs S. L. H.Verified BuyerI recommend this productRated 5 out of 5 stars2 months agoI slept better than I have for a long time.
It does what it says for me.
Was this helpful? - JDJeanette D.Verified BuyerI recommend this productRated 5 out of 5 stars2 months agohaving good nights
it seems to be working having better nights sleep
Was this helpful?
Discover more on The Better Menopause edit
Can sage help with menopause symptoms?
We assess the evidence for potential benefits, look at different ways to take sage and explain what the numbers on the supplements labels really mean.
Read morePerimenopause and menopause skin: Why it feels dry, itchy and breaks out
Perimenopause and menopause can feel like your skin has developed a mind of its own. One day it’s dry and sensitive, the next you’re dealing with unexpected breakouts, something many of us haven’t seen since our teenage years. The good news: these changes are completely normal. With the right support, your skin can feel calm, comfortable and confident again. Why Your Skin Changes in Perimenopause and Menopause As you enter perimenopause, your hormones begin to shift, particularly oestrogen, progesterone and testosterone. Your skin produces less collagen and fewer natural oils. As the skin barrier weakens, moisture escapes more easily, which can lead to sensitivity, irritation, redness, dryness and itching. Fluctuating hormones can also ramp up oil production, causing breakouts around the jawline and chin, inflammation and congestion. It’s not your imagination. Your skin is genuinely behaving differently. Even if your skin feels dry on the surface, it can still be producing excess oil underneath, leading to congestion. That’s why it’s so important to tune into your skin and understand what it actually needs. What Else Affects Your Skin in Midlife Alongside hormone shifts, several other factors influence how your skin looks and feels: Stress, which raises cortisol and stimulates more oil production, triggering breakouts Nutrition and hydration Exercise and sleep quality Environment, pollution and allergens Medication and genetics How to Support Your Skin Through Perimenopause Choose skincare your skin actually needs, not what’s trending Keep your routine simple and consistent Avoid switching products often Be patient. Give any new product at least three months to show a difference If skincare burns, stings or irritates your skin, stop using it Moisturise and hydrate from the inside out. Drink plenty of water and nourish your skin with nutrients that support repair, hydration and glow Don’t wait until bedtime. Support your skin throughout the day How Skin:Genius Supports Skin in Midlife Skin:Genius uses proven active botanical ingredients formulated to work with your skin through the changes of perimenopause and menopause. With consistent use, it can: Help boost collagen and plump the skin Deeply nourish dry skin Improve firmness and radiance for a brighter complexion Reduce unwanted bacteria that trigger breakouts Calm inflammation, redness and soreness Soothe, smooth and even skin tone Deliver visible improvements With the support of Skin:Genius, you can feel confident in your skin again. Competition Inside Out: The Better Menopause × Skin:Genius Win a Skin & Gut Health Bundle Worth £280 Real change starts from the inside out. And this prize is designed to support exactly that. We’ve teamed up with Skin:Genius to give one lucky winner a bundle that works on both fronts, your gut health and your skin, because during perimenopause the two are more connected than most people realise. The prize includes: A Skin:Genius goody bag worth £130 (100% natural, award-winning skincare formulated for skin that’s changing) A £150 voucher to spend with The Better Menopause Enter the competition → Competition closes midnight, 1st May 2026. UK residents only, 18+. Frequently Asked Questions Why does my skin feel so different during perimenopause? Falling oestrogen reduces collagen production and weakens your skin barrier, so moisture escapes more easily. At the same time, shifting testosterone can increase oil production and trigger breakouts. These combined changes are why skin can feel dry, sensitive and congested all at once. Why am I breaking out in my 40s and 50s? Hormonal breakouts in perimenopause usually appear around the jawline and chin. They’re driven by fluctuations in oestrogen and testosterone, and made worse by raised cortisol from stress. This isn’t the same as teenage acne, and it often responds better to gentle, barrier-supportive skincare than to harsh treatments. How long before I see results from new skincare? Give any new product at least three months of consistent use. Skin cell turnover slows with age, so visible changes take longer than they did in your twenties. Switching products frequently can actually worsen sensitivity. Can I support my skin from the inside? Yes. Skin health is shaped by hydration, nutrition, sleep and stress levels. Drinking enough water, eating a nutrient-rich diet and supporting your body with targeted supplements can all help your skin look and feel better through perimenopause and menopause. About the author
Read moreMenopause rage: why you’re feeling so angry
Discover what’s behind those sudden outbursts of rage that really don’t feel like you – and what you can do to help manage your anger.
Read moreWhy Can't I sleep during perimenopause? causes, symptoms and what actually helps
Reviewed by Jo Lyall, Nutritional Therapist (Dip Nut, mBANT, CNHC) and Dr Shahzadi Harper, Resident Doctor at The Better Menopause If you've always been a good sleeper and perimenopause has changed that — you're not imagining it. Sleep disruption is one of the most common symptoms of the menopause transition, affecting up to 60% of women. And it's not just about hot flushes. Hormonal changes during perimenopause affect your brain chemistry, your body clock and your ability to fall and stay asleep in ways that can feel completely bewildering. In this article, we explain why perimenopause affects sleep, what's happening in your body when you wake at 3am, and the evidence-based steps — from nutrition and lifestyle changes to supplements and HRT — that can genuinely help. Key takeaways Sleep disruption during perimenopause affects up to 60% of women and has clear hormonal causes — it's not just stress or ageing Declining oestrogen reduces melatonin production, while falling progesterone lowers GABA activity — both directly affect your ability to fall and stay asleep The common 3am wake-up is often caused by an early cortisol surge, compounded by night sweats and circadian rhythm changes Your gut produces 95% of your body's serotonin (a precursor to melatonin), making gut health an overlooked route to better sleep Evidence-based strategies that help include: morning light exposure, magnesium-rich nutrition, regular movement, targeted supplements, HRT and CBT-I In this article How perimenopause affects sleep Common perimenopause sleep symptoms What actually helps: evidence-based strategies When to see your GP The bottom line How perimenopause affects sleep Sleep problems during perimenopause aren't caused by one thing. They're the result of several overlapping hormonal, neurological and lifestyle factors — which is why they can feel so hard to pin down. Oestrogen, progesterone and your sleep-wake cycle Oestrogen and progesterone do far more than regulate your menstrual cycle. They also influence neurotransmitters that directly affect sleep. Oestrogen helps regulate serotonin and melatonin — two chemicals essential for mood, relaxation and your body's natural sleep-wake rhythm (your circadian rhythm). When oestrogen fluctuates and declines during perimenopause, melatonin production can drop, making it harder to fall asleep and stay asleep. Progesterone enhances the activity of GABA, a calming neurotransmitter that promotes relaxation and sleepiness. As progesterone declines — often one of the earliest hormonal shifts in perimenopause — you may notice more difficulty winding down, more anxiety at bedtime and lighter, more fragmented sleep. Hot flushes and night sweats Vasomotor symptoms — hot flushes and night sweats — are experienced by more than 80% of women going through menopause. They're caused by changes in the brain's thermoregulatory centre, which becomes more sensitive to small shifts in body temperature as oestrogen declines. Night sweats can wake you suddenly, leave you drenched and uncomfortable, and make it difficult to return to sleep. Interestingly, research suggests that many women actually wake just before a hot flush occurs, rather than being woken by it — indicating that the underlying hormonal disruption is affecting sleep architecture directly. The 3am wake-up: cortisol and circadian rhythm changes One of the most commonly reported sleep complaints during perimenopause is waking between 2am and 4am — often with a racing heart or a feeling of anxiety. This is frequently linked to a shift in cortisol patterns. Cortisol, your body's primary stress hormone, normally rises gradually in the early morning to prepare you for waking. During perimenopause, this cortisol surge can happen earlier and more abruptly, pulling you out of deep sleep and leaving you alert and wired. Declining oestrogen also affects the circadian rhythm itself. Research published in the journal Climacteric found that menopause is associated with a significant reduction in melatonin levels, which can weaken the body's internal clock and make you more sensitive to disruptions — including light, noise and temperature changes. Anxiety, mood changes and the racing mind Sleep problems during perimenopause don't always start in the bedroom. Many women experience new or heightened anxiety during this transition — sometimes as a physical sensation (racing heart, chest tightness, a sense of dread) rather than a recognisable worry. The Royal College of Psychiatrists' 2026 Position Statement on menopause and mental health highlighted that only 21% of UK adults are aware menopause can be associated with the onset of new mental health conditions. This means many women — and their GPs — don't connect the dots between mood changes, anxiety and sleep disruption. If your mind races at night or you wake with a jolt of adrenaline, hormonal changes may be driving this — not just stress. Gut health and sleep: an emerging connection Your gut microbiome plays a larger role in sleep than many people realise. Around 95% of the body's serotonin is produced in the gut, and serotonin is a precursor to melatonin. An imbalanced gut microbiome — common during perimenopause as oestrogen levels affect the estrobolome (the collection of gut bacteria that help metabolise oestrogen) — can therefore directly affect your ability to produce the chemicals needed for restful sleep. Supporting gut health during perimenopause isn't just about digestion. It may also be one of the most overlooked routes to better sleep. Better Gut contains six clinically studied probiotic strains designed to support the gut-hormone connection during perimenopause and menopause. Find out more → Common perimenopause sleep symptoms Not sure whether your sleep problems are related to perimenopause? Here are some of the most commonly reported patterns: Difficulty falling asleep, even when tired Waking in the early hours (typically between 2am and 4am) and being unable to get back to sleep Night sweats that disrupt sleep, sometimes multiple times per night Lighter, more fragmented sleep — feeling like you never reach deep sleep Waking feeling unrefreshed, regardless of how many hours you've been in bed Increased anxiety or a sense of dread around bedtime Restless legs or an uncomfortable urge to move your legs at night Needing to use the bathroom more frequently during the night (nocturia) If you're experiencing one or more of these regularly, it's worth speaking to your GP or a menopause-informed healthcare provider. What actually helps: evidence-based strategies for better sleep during perimenopause 1. Prioritise your circadian rhythm Your body's internal clock becomes more fragile during perimenopause, so supporting it with consistent daily cues is one of the most effective things you can do. Get morning light exposure within 30 minutes of waking — even on overcast days, outdoor daylight is significantly stronger than indoor lighting and helps reset your circadian rhythm Keep a consistent wake time, even at weekends — this anchors your body clock more effectively than a consistent bedtime Reduce bright light and screens in the evening — dim your home lighting after 8pm and consider blue-light-blocking glasses if you use screens at night 2. Support your nutrition What and when you eat can have a meaningful impact on sleep quality. Eat a balanced evening meal with protein, healthy fats and fibre-rich carbohydrates to prevent blood sugar dips overnight — these dips can trigger cortisol spikes that wake you in the early hours Include magnesium-rich foods such as dark leafy greens, pumpkin seeds, dark chocolate and almonds — magnesium supports muscle relaxation, nervous system calm and sleep quality, and many women become depleted during perimenopause Consider foods that support melatonin production — tart cherries (such as Montmorency cherries), walnuts, oats and bananas all contain compounds that may support your body's natural melatonin levels Avoid caffeine after midday and limit alcohol, which may help you fall asleep initially but fragments sleep in the second half of the night 3. Move your body — but time it well Regular physical activity is one of the strongest evidence-based interventions for improving sleep quality. Research consistently shows that women who exercise regularly fall asleep faster and experience deeper, more restorative sleep. Aim for at least 30 minutes of moderate activity most days — walking, swimming, strength training and yoga are all beneficial Morning or early afternoon exercise supports circadian rhythm alignment Avoid intense exercise within 2–3 hours of bedtime, as it can elevate cortisol and delay sleep onset 4. Support your gut health Given the gut-brain connection and the role of the microbiome in producing serotonin and melatonin, supporting gut health can be a meaningful part of a sleep strategy during perimenopause. Eat a diverse range of plant-based foods — aim for 30 different plant foods per week to support microbial diversity Include fermented foods such as live yoghurt, kefir, sauerkraut and kimchi Consider a targeted probiotic designed for women in perimenopause, containing clinically studied strains that support the gut-hormone axis 5. Create a sleep-supportive environment Small changes to your sleeping environment can make a significant difference, particularly if night sweats are an issue. Keep your bedroom cool — between 16°C and 19°C is ideal Use breathable, natural-fibre bedding (cotton or linen) and consider layering so you can adjust easily Make your room as dark as possible — blackout curtains or an eye mask can help, especially as the mornings get lighter Remove or turn away clocks — research shows that clock-watching during the night increases anxiety and makes it harder to return to sleep 6. Explore targeted supplements Several supplements have evidence for supporting sleep during perimenopause. For a deeper look at the research, see our guide to natural remedies for menopause sleep problems. Always consult your healthcare provider before starting a new supplement, particularly if you take other medications. Magnesium glycinate — well-absorbed and supportive of muscle relaxation, nervous system calm and sleep quality Ashwagandha (KSM-66) — an adaptogenic herb shown in clinical studies to reduce cortisol and improve sleep quality Saffron — emerging research suggests saffron may support mood, reduce anxiety and improve sleep in menopausal women Montmorency cherry — a natural source of melatonin that may support your body's sleep-wake cycle Chamomile — contains apigenin, an antioxidant that binds to receptors in the brain to promote relaxation Better Night combines KSM-66 Ashwagandha, saffron, magnesium, chamomile and Montmorency cherry to help you fall asleep faster, stay asleep longer and wake up clearer. Find out more → 7. Consider HRT For many women, hormone replacement therapy (HRT) can significantly improve sleep by addressing the root cause: declining oestrogen and progesterone. HRT has been shown to reduce hot flushes and night sweats, improve mood and anxiety, and support more restful, consolidated sleep. If you're experiencing moderate to severe sleep disruption during perimenopause, it's worth discussing HRT with a menopause-informed healthcare provider who can assess your individual risk profile and help you make an informed decision. For more on hormonal and non-hormonal options, read our guide to alternatives to HRT. 8. Try cognitive behavioural therapy for insomnia (CBT-I) CBT-I is recommended by NICE as a first-line treatment for insomnia and has been shown to be effective for menopause-related sleep problems. It works by addressing the thoughts and behaviours that perpetuate poor sleep — such as spending too long in bed, worrying about not sleeping, and developing unhelpful associations between your bed and wakefulness. CBT-I can be accessed through your GP, a sleep clinic, or digital programmes such as Sleepio (available free via the NHS in some areas). When to see your GP If sleep problems are significantly affecting your daily life, your mood or your ability to function, don't wait — seek support. This is particularly important if you're experiencing: Persistent insomnia lasting more than three months Symptoms of sleep apnoea (loud snoring, gasping or choking during sleep, excessive daytime sleepiness) Significant anxiety or depression alongside sleep disruption Night sweats that don't respond to lifestyle changes Your GP can help identify whether your sleep problems are related to perimenopause, another underlying condition, or both — and can discuss treatment options including HRT, medication and referral to specialist services. The bottom line Sleep disruption during perimenopause is real, it's common, and it has clear hormonal and physiological causes. You're not failing at sleep — your body is going through a significant transition, and the systems that regulate your rest are being affected. The good news is that there are practical, evidence-based steps you can take — from supporting your circadian rhythm and nutrition to exploring supplements, HRT and CBT-I. Small, consistent changes can make a meaningful difference. If perimenopause has changed how you sleep, you don't have to just push through it. Support is available, and better nights are possible. This article is for informational purposes and is not a substitute for professional medical advice. If you have concerns about your sleep or menopause symptoms, please speak to your GP or a qualified healthcare provider. Related reading How menopause causes sleep problems — and what you can do 6 natural remedies for menopause sleep problems Magnesium for menopause: benefits, which type is best, dosage Alternatives to HRT: natural options and other medications Probiotics for menopause: which strains really help? About the author
Read moreBrain Fog made me forget the route to work. Then it made me leave my career.
Sarah Stevens, 48, was a teacher for 21 years before perimenopause brain fog forced her to walk away from the career she loved. Here, she shares how supporting her gut health helped her find clarity, confidence and a completely new path. The moment everything changed I was driving to school one morning, following the same route I had taken every weekday for the past 10 years, when suddenly my mind went completely blank. I was approaching a junction I knew by heart. A turn I could normally do on autopilot. And yet I could not remember whether I needed to go left or right. I slowed the car, heart pounding, staring at the road ahead as panic washed over me. Left or right. I asked myself the question again and again, willing the answer to come. It did not. I sat there gripping the steering wheel, convinced something was seriously wrong. This was not forgetfulness. This was not stress. This felt frightening and unfamiliar. 21 years of loving my job I am a teacher, or at least I was. Teaching had been my life for 21 years. I loved the students, the rhythm of the school year and the sense of purpose it gave me. I have two teenage children, a busy family life, and I had always been organised, articulate and confident. Then perimenopause arrived. Quietly at first, and then all at once. When brain fog takes your words The brain fog was the most frightening part. During parent-teacher meetings, I would open my mouth and completely lose the word I needed. Simple words. Everyday language. I would forget pupils' names mid-conversation or struggle to describe their work clearly. Inside, I was terrified. Outwardly, I was mortified. At the same time, my health was deteriorating in other ways. I have lived with colitis for years, but during perimenopause it flared badly. Constant inflammation, urgency and exhaustion left my gut feeling permanently unsettled. I went to my GP and was supported with medication for my colitis. Whilst this helped a great deal with my symptoms, perimenopause symptoms like brain fog lingered and my anxiety never really went away. The hardest decision of my life It became clear to me that teaching, at least in the way I had always done it, was not a job I could continue while feeling like this. The cognitive load, the pace, the constant decision-making and the pressure of being "on" all day were simply too much. In February 2025, I made the hardest decision of my life. I resigned from my role. I officially left the profession in April 2025. Walking away from a career I loved after 21 years felt like grief. But I was so embarrassed by my cognitive symptoms that I could not face another term of meetings, lesson planning or standing in front of a classroom pretending everything was fine. I told people I needed a change. The truth was, I did not trust my own mind anymore. Finding the right support As I began trying to feel better, I realised something important. I did not want to leave education or helping people behind. I just needed a role that was less demanding, more focused and more sustainable for where I was physically and mentally, but where I could still make a real difference. That was when I sought specialist support from a menopause specialist, who took a much more holistic view of what was happening to me. She explained that perimenopause affects the entire body, including the brain, gut and nervous system, and that supporting these systems together was key. She helped me understand how hormonal fluctuations can disrupt gut health, sleep and cognition, and how this can show up as anxiety, inflammation and brain fog. Small, practical changes She suggested a number of practical, manageable changes. I was encouraged to increase protein-rich foods to support energy and concentration, and to include more omega-3-rich foods to help with inflammation and brain health. I was advised to cut back on sugar and alcohol, which can worsen anxiety, sleep disruption and gut symptoms. Sleep became a priority. She explained the role of magnesium-rich foods and the importance of a calmer, more consistent bedtime routine to help regulate the nervous system. Gentle movement rather than intense exercise was encouraged, alongside proper rest without guilt. The gut-hormone connection She also explained the crucial role of gut health in hormone regulation, particularly a group of bacteria known as the estrobolome, which helps process and regulate oestrogen in the body. If the gut is out of balance, hormone symptoms such as brain fog, anxiety and inflammation can worsen. As part of this wider approach, she recommended Better Gut, a probiotic designed specifically for women in perimenopause, to support gut health alongside dietary changes. None of it felt extreme. It felt achievable. So I started to make a few of these small changes every day. What shifted I started taking one capsule of Better Gut probiotic once a day, alongside more movement (walking daily, some simple strength exercises), less sugar and alcohol, and added protein. Simple swaps like having eggs for breakfast and salmon for dinner. After about three weeks, something shifted. My colitis symptoms were less noticeable. The constant inflammation settled and my digestion felt calmer than it had in months. But what surprised me most was my mental clarity. The brain fog began to lift. I could find words again. I felt less anxious and more grounded. I was not suddenly a different person, but I felt more like myself for the first time in over a year. A new career, a better life As my confidence returned, I felt ready to think about work again. I knew I still wanted to support families and children, just in a way that felt manageable and meaningful. I now work as a neurodiversity family support practitioner, supporting children and parents more closely on an individual basis. The pace and pressure is not like teaching, but I feel like I make a real difference. I love my new job. I feel calmer, more present and more fulfilled than I did before. In many ways, I am happier now than I ever was in my teaching career. Looking back, perimenopause did not end my career. It changed it for the better. What I wish more women knew All is not lost when perimenopause hits. With the right medical guidance, alongside natural and practical support, there is a plan. There is another way of looking at this stage of life that can be stabilising, empowering and genuinely life-changing. I did not lose my mind. I found a new way forward. Better Gut is a daily probiotic formulated specifically for women in perimenopause and menopause. It contains six clinically studied bacterial strains chosen to support the gut-hormone connection, ease digestive discomfort and help restore balance from the inside out. If you are experiencing persistent memory loss, brain fog or cognitive changes, please speak with your GP or a menopause-informed healthcare provider. These symptoms are common in perimenopause but should always be checked. About the author
Read moreStrength training during perimenopause: What actually matters and where to start
Perimenopause and menopause mark a significant transition in a woman’s life. As hormone levels fluctuate and eventually decline, the body can go through a range of physical and emotional changes. Energy levels may shift, sleep can become disrupted, and exercise routines that once worked may suddenly feel less effective. At Amp Wellbeing, the belief is simple: consistent, supportive movement is one of the most powerful ways to help women navigate these shifts. Strength training does not need to be intense or complicated. What matters most is building a routine that feels sustainable; small, regular sessions that support muscle health, mobility and long-term wellbeing. With the right approach to nutrition, movement and recovery, this stage of life can become one where women build resilience and confidence in their bodies. Strength training, in particular, plays a key role in supporting the body through the hormonal changes of perimenopause and beyond. Understanding the Hormonal Shift Perimenopause, the transitional period leading up to menopause, typically begins in a woman’s mid-40s, although it can start earlier. During this phase, oestrogen and progesterone begin to fluctuate before gradually declining. These hormonal changes can cause symptoms such as hot flushes, sleep disturbances, brain fog and mood shifts. Menopause is defined as the point when a woman has gone 12 months without a menstrual cycle. The reduction in reproductive hormones can affect everything from bone density to metabolism. One of the most important physiological changes during this stage is the gradual loss of muscle mass. Research suggests muscle mass can decline by 3–8% per decade after the age of 30, with this loss accelerating as oestrogen levels decrease. This is why strength training becomes particularly valuable during perimenopause. Why Strength Training Matters Muscle plays a vital role in supporting overall health, far beyond simply shaping the body. Maintaining lean muscle mass helps protect bone density, improve balance and stability, and support a healthy metabolism. Muscle tissue is metabolically active, meaning it helps the body burn energy even at rest. As muscle mass declines, metabolic rate can also decrease, which is one reason weight gain can become more common during midlife. Strength training helps counteract this process by stimulating muscle growth and preserving bone density. Studies show that resistance training can slow age-related muscle loss and support stronger bones, reducing the risk of fractures and osteoporosis later in life. Training Smarter During Perimenopause When exercise results begin to plateau, it can be tempting to increase intensity or add more cardio. However, during perimenopause many women benefit more from training smarter rather than harder. Hormonal changes can increase sensitivity to stress and raise cortisol levels. Excessive high-intensity training may therefore leave the body feeling more fatigued rather than energised. Instead, a balanced routine that prioritises strength training, moderate cardio and adequate recovery tends to work best. Experts often recommend two to three strength sessions per week. These do not need to be long or overly intense. Consistency is far more important than pushing to exhaustion. For many women, building a simple routine at home can make strength training easier to maintain. A comfortable surface such as a supportive exercise mat can create a dedicated space for movement, while small tools like wrist weights or weighted balls can add gentle resistance without the need for heavy equipment. Nutrition That Supports Strength Exercise is only one part of supporting the body through menopause. Nutrition also plays a key role. Protein becomes particularly important during midlife, as it helps repair and maintain muscle tissue. Many experts suggest aiming for roughly 0.8–1.2 grams of protein per kilogram of body weight each day. Bone health also becomes a priority. Nutrients such as calcium and vitamin D help maintain bone density and reduce the risk of osteoporosis. These can be found in foods such as leafy greens, dairy products, fortified foods and oily fish. Healthy fats, particularly omega-3 fatty acids from foods like flaxseeds, walnuts and fish, can support heart health and help reduce inflammation. Meanwhile, limiting highly processed foods and excess sugar may help stabilise energy levels and mood. The Role of Recovery Recovery becomes increasingly important during perimenopause. Strength training works by creating small micro-tears in muscle fibres, which then repair and grow stronger during rest. Spacing workouts across the week allows the body time to adapt and rebuild. Active recovery activities such as walking, gentle yoga or Pilates can help improve mobility and reduce muscle soreness. Hydration is also important, particularly as symptoms such as hot flushes and night sweats can increase fluid loss. Where to Start For those new to strength training, starting simple is often the most sustainable approach. Strength training doesn’t require a gym membership or heavy equipment. Many women begin with short sessions at home, gradually building confidence and strength over time. A beginner routine might include movements such as squats, glute bridges, rows and shoulder presses. These compound exercises work multiple muscle groups and provide the most benefit in a short amount of time. Adding light resistance through bands, wrist weights or small weighted balls can gradually increase strength while keeping movements controlled and safe. If you’re unsure where to begin, try this simple routine two or three times a week: Squats – 10 repetitionsStrengthen the legs and glutes while supporting bone health. Glute bridges – 10 repetitionsActivate the glutes and support lower back stability. Shoulder presses – 10 repetitionsUsing light resistance such as wrist weights or small hand weights. Bent-over rows – 10 repetitionsHelp strengthen the upper back and improve posture. Core stability (plank or dead bugs) – 30 secondsStrengthens the deep muscles that support the spine and pelvis. Repeat the circuit two to three times, resting briefly between each round. A supportive surface such as a comfortable exercise mat can make floor-based exercises easier, while light resistance tools like wrist weights or weighted balls allow you to gently increase intensity as your strength improves. Even two short sessions per week can begin to build strength and confidence. Over time, resistance or repetitions can gradually increase as the body adapts. Consistency Over Perfection Perhaps the most important takeaway is that consistency matters more than intensity. Small, regular strength sessions can have a powerful cumulative effect, helping to maintain muscle mass, support bone health and improve energy levels over time. Perimenopause is not the end of strength. In many ways, it can be the beginning of a new approach to movement, one focused less on pushing harder and more on building lasting strength, resilience and wellbeing. Enter Our Competition with Amp Wellbeing Win a Movement & Wellbeing Bundle Worth Over £300 To celebrate the arrival of spring, The Better Menopause has teamed up with AMP Wellbeing to give one lucky winner a bundle designed to help you feel strong, supported and confident in your body. The prize includes AMP Wellbeing’s beautifully designed Complete Movement Set (worth £152) and a £150 voucher to spend with The Better Menopause. Tap here to enter
Read moreMenopause and sleep: 6 natural ways to beat 3am wake-ups
In this guide Why can't I sleep during menopause? Declining oestrogen and progesterone Elevated cortisol at night Poor gut health and melatonin production 6 natural remedies for menopause insomnia Support your sleep from the inside out Frequently asked questions References Restless nights. 3am wake-ups. That frustrating "wired but tired" feeling that no amount of herbal tea seems to fix. If this sounds familiar, you're not imagining it — and you're far from alone. Millions of women going through perimenopause and menopause struggle with disrupted sleep, and the causes run deeper than most people realise. Hormonal shifts, elevated stress hormones, and an imbalanced gut microbiome can all quietly sabotage your ability to fall asleep, stay asleep, and wake up feeling rested. In this evidence-based guide, we explain exactly why menopause disrupts sleep — and share six proven, natural strategies to help you reclaim restful nights. Why Can't I Sleep During Menopause? The Root Causes Menopause insomnia is primarily driven by three physiological changes: declining oestrogen and progesterone (which regulate your sleep cycle and body temperature), elevated evening cortisol (which keeps your nervous system alert), and disrupted gut health (which reduces production of melatonin, your body's natural sleep hormone). 1. Declining Oestrogen and Progesterone As oestrogen and progesterone fluctuate and decline during perimenopause and menopause, your sleep architecture changes significantly. Oestrogen helps regulate your circadian rhythm and core body temperature. When levels drop, hot flushes and night sweats become more frequent — two of the most common triggers for broken sleep during menopause. Progesterone is your body's natural calming hormone. It promotes deep, restorative sleep. As production slows, sleep tends to become lighter, more fragmented, and less refreshing. 2. Elevated Cortisol at Night Hormonal changes combined with the cumulative stress of midlife can push cortisol levels higher in the evening — exactly when they should be falling. The result? A nervous system that won't switch off, making it harder to relax, drift off, or stay asleep through the night. 3. Poor Gut Health and Melatonin Production Here's one most women don't expect: your gut plays a direct role in sleep. Around 95% of your body's serotonin is produced in the gut, and serotonin is the precursor to melatonin — your primary sleep hormone. When your gut microbiome is out of balance, melatonin production can suffer, and so does your sleep cycle. This connection between menopause and gut health is one of the most overlooked — and most actionable — pieces of the sleep puzzle. 6 Natural Remedies for Menopause Insomnia 1. Lower Cortisol With an Evening Wind-Down Routine A structured wind-down helps signal to your nervous system that it's safe to rest. Try building a 30–60 minute buffer before bed that includes mindfulness or deep breathing exercises, restorative yoga or gentle stretching, and switching off screens at least 60 minutes before sleep. Consistency matters here — the more predictable your routine, the more effectively your body responds. 2. Create a Sleep-Optimised Bedroom Your sleep environment can make or break your night — especially if you're dealing with menopause night sweats. Keep your bedroom cool (around 16–18°C), dark, and quiet. Invest in blackout blinds and breathable, natural-fibre bedding. Dim overhead lights after sunset and reduce blue light exposure from phones and laptops in the evening. 3. Exercise Daily — But Time It Right Regular physical activity is one of the most effective natural sleep aids during menopause. However, high-intensity workouts after 6pm can spike cortisol and leave you wired at bedtime. Aim for movement earlier in the day — walking, Pilates, swimming, or yoga are all excellent choices that support sleep without overstimulating your system. 4. Support Your Gut Microbiome for Better Sleep Because your gut is so closely linked to serotonin and melatonin production, improving your microbiome health can have a noticeable impact on sleep quality. This is especially relevant during perimenopause, when hormonal fluctuations disrupt the delicate balance of your gut bacteria. Better Gut is a daily probiotic designed to support digestion, mood, and sleep. It contains six clinically studied strains — including Lactobacillus rhamnosus and Bifidobacterium lactis — shown to help reduce cortisol and promote a healthier, more balanced microbiome. Learn more about Better Gut → 5. Nourish Your Nervous System With Targeted Nutrients Hormonal stress can deplete the key vitamins and minerals your body needs to wind down and recover overnight. Without them, even good sleep habits may not be enough. Better Night is a gentle, non-habit-forming supplement formulated to help you fall asleep faster, stay asleep longer, and wake up clear-headed. It combines KSM-66® Ashwagandha, Affron® Saffron, Chamomile, Magnesium, Montmorency Cherry, and Vitamins B6, B12, D3 & K2 — all chosen for their evidence-based role in supporting relaxation and sleep. Learn more about Better Night → 6. Explore Mind–Body Therapies Calming the mind is just as important as calming the body. Guided meditation and body scan exercises before bed, a gratitude journal to process the day's thoughts, and sleep-specific breathing exercises or calming soundscapes can all help lower sympathetic nervous system activity — making it easier to transition into deep, restorative sleep. Support Your Sleep From the Inside Out If you're ready to address the root causes of menopause-related sleep problems — not just the symptoms — a combined approach works best. Pairing Better Gut and Better Night targets the three biggest drivers of menopause insomnia: gut health, cortisol balance, and hormonal shifts. Our Serenity Bundle brings both formulas together in one simple daily routine, helping you: Balance your gut microbiome Lower night-time cortisol Support your natural sleep–wake rhythm Because better nights mean better days. And you deserve both. Shop the Serenity Bundle → Frequently Asked Questions About Menopause and Sleep Why do I wake up at 3am during menopause? Waking at 3am during menopause is often caused by a drop in progesterone (which promotes deep sleep), a spike in cortisol during the second half of the night, or night sweats triggered by declining oestrogen. Addressing cortisol balance and supporting your nervous system can help you sleep through. Does gut health affect sleep during perimenopause? Yes. Around 95% of your body's serotonin is made in the gut, and serotonin converts to melatonin — your primary sleep hormone. During perimenopause, hormonal fluctuations can disrupt gut bacteria balance, which in turn reduces melatonin production and worsens sleep quality. What is the best natural supplement for menopause insomnia? Evidence-backed natural ingredients for menopause insomnia include magnesium, ashwagandha (especially KSM-66®), saffron extract, chamomile, and montmorency cherry. A targeted supplement combining these with B vitamins and vitamin D3 can support relaxation and healthy sleep-wake cycles without habit-forming ingredients. How long does menopause insomnia last? Menopause-related sleep disruption varies between women. Some experience it for a few months during perimenopause, while others deal with it for several years into post-menopause. The good news is that targeted lifestyle changes, gut support, and nervous system nourishment can significantly improve sleep quality at any stage. Can probiotics help with menopause sleep problems? Emerging research suggests yes. Specific probiotic strains such as Lactobacillus rhamnosus and Bifidobacterium lactis have been shown to help reduce cortisol and support serotonin production in the gut — both of which play a direct role in sleep quality. A daily probiotic formulated for the gut-sleep connection may help improve sleep during menopause. References Baker FC, de Zambotti M, Colrain IM, Bei B. Sleep problems during the menopausal transition: prevalence, impact, and management challenges. Nat Sci Sleep. 2018;10:73-95. PubMed Hirotsu C, Tufik S, Andersen ML. Interactions between sleep, stress, and metabolism: From physiological to pathological conditions. Sleep Sci. 2015;8(3):143-152. PubMed Li Y, Hao Y, Fan F, Zhang B. The role of microbiome in insomnia, circadian disturbance and depression. Front Psychiatry. 2018;9:669. PubMed Kredlow MA, Capozzoli MC, Hearon BA, Calkins AW, Otto MW. The effects of physical activity on sleep: a meta-analytic review. J Behav Med. 2015;38(3):427-449. PubMed
Read moreWhat causes sore breasts during menopause, and what can help?
We explore the links between hormonal changes and breast pain, both during perimenopause and after menopause, and suggest some approaches that could help.
Read moreCan menopause cause headaches and migraines?
We explore how changing oestrogen levels can make headaches and migraines worse, what these ‘hormone headaches’ can feel like, plus the treatments that could help.
Read moreWhy it’s time to reclaim your pleasure
Did you know that your pleasure matters? I wonder if this flies in the face of the stories you’ve been told about it? Pause for a moment to think here. How do you feel about pleasure, or giving yourself permission to receive it? Let’s consider for a moment the impact that the selfless woman archetype has had on our capacity to experience pleasure… It is time to reclaim your right to receive! There is nothing indulgent or selfish about prioritising it because pleasure is fundamental to healing and navigating stress. Why pleasure is so vital for your health We’re all familiar with the ‘fight or flight’ stress response, I hope you’re also aware of the concept of glimmers, a concept coined by clinician and trauma expert, Deb Dana1. You can think of glimmers as the opposite to threats – these are cues, internal or external, that help you feel joyful, at ease, peaceful, or safe and you need them for your health. Glimmers shift your nervous system out of the stress response and into the ventral vagal state of ‘rest and digest’, allowing you to do exactly that – to heal and assimilate the nourishment available to you, resourcing you to cope with life’s demands. Far from frivolous, your health depends on it. Glimmers help you heal, boost your immune function, provide you with pain relief, and promote better sleep. Pleasure lifts your mood, replenishes your energy levels, helps you recover from stress, alleviates worry and facilitates better creative planning and problem solving. Glimmers give shape and potentially meaning to your life, enhancing motivation and staying power, but do watch out for short term pleasure with longer term costs! They can also deepen your bonds, allowing for shared humanity, connection and memory making. Being open to glimmers into your life How can you give yourself permission to experience more pleasure? How would you like to receive pleasure? What feels pleasurable to you? Enjoy pondering, and if you feel stuck, I’ve got you covered below: Feeling the sunlight on your skin Listening to bird song Watching a sunset Enjoying a hug Seeing the reflection of sunlight on water Feeling the warmth and comfort of a blanket Imbibing the scent and warm glow of a candle Sitting with the cat on your lap Wrapping your hands around a warm cup of tea Receiving pleasure via your body You don’t have to wait for the next rainbow to appear to experience pleasure, you can deliberately seek it out. Perhaps the source you’re looking for is within fingertips reach... When was the last time you turned to your body to seek pleasure? Perhaps you’re thinking I haven’t got the appetite for that… It’s not you, it’s a function of energy. Depleted or struggling with the weight of mental load? It is no surprise that sexual desire is low. Close some mental tabs, maybe reapportion some responsibility, have a rest to replenish and see what blooms. Darling, it is time to get your mojo back. Now that you are aware of all the beautiful benefits of pleasure, I hope it can get bumped back up your list of priorities. Find some quiet time to explore you again. Half the battle is just getting reacquainted again. Raising kids, perimenopause, you might feel like it’s been a long time since you felt alive ‘down there’, or like it’s not really yours anymore. If sex has felt like an act to please someone else or if the orgasm gap has made sex feel like a chore, give yourself time to shift gears and allow a different purpose to guide you. It needn’t be sexual, there are all sorts of ways we can turn to the body for pleasure. It might be nice to just cradle your chin in your hands and feel held or massage some magnesium oil into your feet before sleep. Maybe you just want to wrap up in a weighted blanket and cocoon yourself. The invitation is to go where you feel drawn and honour yourself. What to do when you feel guilty for seeking pleasure Darling, those tales you have been told about pleasure, please can you question whether this ethos serves you and gently reflect on what it has cost you? Can you give yourself permission to make different choices moving forwards? What is the purpose of pleasure? It’s not just a nice to have! If good sleep, a healthy immune system, resilience, access to patience and a buoyant mood matter to you, then here is the invitation to prioritise life-giving pleasure! Let glimmers move you out of the stress response into the healing, empathetic state of rest and digest mode, helping you not only feel safe but to be a calm, safe place for those you love. If you reflect on some peak life moments of awe, joy or contentment, times you felt alive, what cultivated them? Were there some you enjoyed solo? Which did you relish with others? Have they provided rich memories that still feed you now? Who benefitted from this joy (not just in the moment but in the beautiful afterglow). Please can you write down your thoughts now on why it is ok for you to experience pleasure in your life? If there are still barriers, I get it, they can be tenacious… says who? What does your ‘future self’ think? Can pleasure help you commit to some healthy habits? What kind of pleasure would you like your loved ones to embrace? Why are you any different? Make your mind map of life-giving joy bringers now, thinking along the lines of your senses, movement, meaning, nature, learning, and connection. Choose one now darling and savour it. You are worthy and even if you don’t feel worthy yet, I invite you to do it anyway. Notice how you feel afterwards and the benefits it brings to all you love. References Dana D. The Polyvagal Theory in Therapy: Engaging the Rhythm of Regulation. First edition. W.W. Norton & Company; 2018.
Read moreIs it normal? perimenopause symptom faqs - irregular bleeding, itching, spotting + more
If you’ve ever found yourself thinking, “Is this perimenopause… or is something wrong with me?” you’re not alone. Perimenopause can feel confusing because symptoms can appear, disappear, and change intensity month to month. Hormones don’t decline in a straight line here — they fluctuate. This post answers the real questions women search for (especially when symptoms feel unexpected), plus gentle guidance on what’s common, what to track, and when it’s worth checking in with a clinician. For a trusted overview of menopause symptoms, see: Menopause symptoms (NHS). Quick Navigation Is irregular bleeding normal in perimenopause? Is spotting during perimenopause normal? Is itching a perimenopause symptom? Is feeling flat or unmotivated normal? Is sudden anxiety or panic normal? Is heart racing or palpitations normal? Is waking up at 3am a perimenopause thing? Is brain fog normal in perimenopause? Is joint pain or stiffness normal? Is weight gain around the middle normal? Is feeling “not like myself” normal? Other “is this normal?” symptoms When a symptom might not be normal How to track symptoms without obsessing Is irregular bleeding normal in perimenopause? Yes. Irregular bleeding is very common in perimenopause. Ovulation becomes less predictable, and fluctuating oestrogen and progesterone affect how the uterine lining builds and sheds. You might notice: Shorter or longer cycles Heavier or lighter bleeding Skipped periods Bleeding that starts and stops Bupa’s UK menopause guidance explains bleeding changes and when to get checked here: Bleeding during perimenopause (Bupa UK). Is spotting during perimenopause normal? Spotting can be normal during perimenopause, particularly when hormones fluctuate and the uterine lining sheds unevenly. Spotting may occur: Between periods Around ovulation After a missed period Helpful rule of thumb: Occasional light spotting can be part of the transition, but spotting that is persistent, heavier than expected, happens after sex, or feels unusual for you should be checked. Further guidance: Spotting and bleeding changes (Bupa UK). Is itching a perimenopause symptom? Yes. Oestrogen helps maintain moisture and elasticity in skin and vaginal tissues. As levels fluctuate and decline, tissues can become drier and more sensitive, leading to itching, irritation, or burning. Itching may show up as: Vaginal or vulvar itching Dry, itchy, or “crawly” skin Increased sensitivity to soaps or fabrics The British Menopause Society describes this under genitourinary syndrome of menopause (GSM): GSM consensus statement (BMS). Is feeling flat or unmotivated normal in perimenopause? Yes. Many women describe feeling emotionally flat rather than sad — a loss of drive, motivation, or enjoyment. Hormonal fluctuations can affect dopamine and serotonin, which influence motivation and reward. You might notice: Little motivation to start things you once enjoyed Feeling emotionally muted or detached Low energy without feeling depressed Poor sleep, chronic stress, and blood sugar swings can make this feel worse. The NHS recognises low mood and anxiety as menopause symptoms: Mood changes in menopause (NHS). Is sudden anxiety or panic normal in perimenopause? It can be. Hormonal changes can affect the nervous system and stress response, making some women more prone to anxiety or panic — even if they’ve never experienced it before. The NHS lists anxiety as a menopause symptom: Anxiety and menopause (NHS). Is heart racing or palpitations normal? Palpitations are commonly reported in perimenopause. Hormonal fluctuations can increase sensitivity to adrenaline and affect how the nervous system regulates heart rhythm. They often occur at night, during stress, or around cycle changes. While they can be hormone-related, heart symptoms can have multiple causes. Guidance from the NHS: Heart palpitations (NHS). Seek urgent care if palpitations occur with chest pain, breathlessness, or fainting. Is waking up at 3am a perimenopause thing? It can be. Perimenopause can disrupt sleep through night sweats, anxiety, and hormonal shifts that affect cortisol (stress hormone) rhythms and blood sugar regulation. Many women report waking between 2–4am with a racing mind. Sleep problems are recognised menopause symptoms by the NHS: Sleep problems in menopause (NHS). Is brain fog normal in perimenopause? Yes. Oestrogen plays a role in memory and cognitive processing. When levels fluctuate, some women notice forgetfulness, word-finding issues, or difficulty concentrating. Poor sleep, stress, and anxiety can intensify brain fog. The NHS includes difficulty concentrating among menopause symptoms: Difficulty concentrating (NHS). Is joint pain or stiffness normal? Yes. Oestrogen helps reduce inflammation and support joint lubrication. As hormone levels fluctuate and decline, inflammation can increase and joints may feel stiffer or more achy. You might notice: Morning stiffness Achy knees, hips, shoulders, or fingers Longer recovery after activity The NHS lists joint pain as a menopause symptom: Joint pain in menopause (NHS). Is weight gain around the middle normal? Yes. Hormonal changes in perimenopause can affect insulin sensitivity, muscle mass, and fat storage patterns — even if diet and exercise haven’t changed. As oestrogen fluctuates, fat storage often shifts toward the abdomen, while age-related muscle loss can slow metabolism. The NHS includes weight gain as a possible menopause symptom: Weight gain in menopause (NHS). Is feeling “not like myself” normal in perimenopause? Yes. Many women describe a shift in confidence, patience, motivation, or emotional steadiness. Mood changes, sleep disruption, and anxiety can all contribute. This experience is common — and temporary for many. Understanding what’s happening can be grounding. Other “is this normal?” perimenopause symptoms Digestive changes, bloating, or IBS-like symptoms Dry or gritty eyes Tingling sensations or “pins and needles” Tinnitus or ear ringing Increased sensitivities to products or fabrics When a symptom might not be normal Very heavy bleeding (soaking pads or tampons hourly) Bleeding after sex Bleeding after 12 months without a period Severe pelvic pain Persistent itching with discharge, odour, or pain NHS guidance on postmenopausal bleeding: Postmenopausal bleeding (NHS). How to track symptoms without obsessing Tracking symptoms can help you spot patterns without overanalysing. A simple weekly check-in is often enough. Cycle changes Sleep quality Mood and motivation Itching or dryness Digestive symptoms Download our symptom tracker A gentle reminder This content is for education and support only and is not medical advice. If symptoms feel severe, persistent, or worrying, please contact a qualified healthcare professional.
Read moreAre there tests for perimenopause or menopause, and how reliable are they?
Can a lab or home test kit really tell you whether you’re in perimenopause or have reached menopause? And are there better ways to get a diagnosis?
Read moreJanuary reset: How berberine can help with menopause weight gain
Explore the science behind berberine, metabolic health and gut support — and why they matter for menopause weight gain in January and beyond.
Read moreIs your itchy skin a menopause symptom, and what can you do to relieve it?
Learn how reduced hormone levels lead to changes to your skin health, plus the medication, creams and supplements that could help.
Read moreMenopause lower back pain: what causes it and what can help?
We explore the links between perimenopause, menopause and lower back pain, and look at some of the approaches that could provide relief.
Read moreThe Estrobolome: Why your gut–hormone connection matters in perimenopause
Discover how your gut microbiome, known as the estrobolome, affects oestrogen balance and perimenopause symptoms — and how to support it naturally.
Read moreWhy frozen shoulder is so common during menopause, and what helps
Learn why frozen shoulder affects midlife women, how menopause impacts joint health, and what you can do to reduce inflammation and recover naturally.
Read moreHow to stay cool during perimenopause: Natural relief for hot fushes, burning feet & hormonal heat
Perimenopause can feel like someone turned up the thermostat on your life. Whether you’re suddenly sweating through your clothes in a meeting or waking in the middle of the night with burning feet and a flushed face, you’re not imagining it. These heat surges aren’t just from the weather—they’re hormonal, and they can hit hard. The classic symptoms of perimenopause—hot flushes and night sweats—are well known. But many women also experience burning sensations in the feet or hands, skin sensitivity, and heat intolerance, especially during the summer months[1]. Why do we overheat during perimenopause? Oestrogen doesn’t just regulate your menstrual cycle—it helps manage body temperature, circulation, and mood. As levels start to fluctuate (often wildly) during perimenopause, your brain can misinterpret small changes as overheating. Cue: sweating, flushing, and restlessness[2]. What’s more, declining oestrogen affects the nervous system and skin, sometimes causing burning feet, tingling hands, or even electric shock–like sensations[3], less common but very real symptoms many women don’t expect. 6 Ways to keep cool, naturally 1. Hydrate intelligently Drink 1.5–2 litres of water daily, and add a pinch of sea salt or a splash of coconut water to restore electrolytes lost through sweating[8]. 2. Cool your feet Soak burning feet in cool (not icy) water with Epsom salts. The magnesium helps ease nerve irritation and relax tense muscles[9]. 3. Wear breathable fabrics Choose loose-fitting clothes made from cotton, bamboo or linen. Avoid synthetic materials which trap heat and can irritate sensitive skin. 4. Use cooling herbs Sage tea, peppermint, red clover, and evening primrose oil have shown promise in reducing hot flushes and night sweats[10]. 5. Prioritise sleep Keep your bedroom cool, dark, and quiet. Try sleeping with a fan, and avoid screens an hour before bed to support natural melatonin production[11]. 6. Mindful movement & rest Exercise helps regulate temperature and stress, but overdoing it can backfire. Try gentle yoga, walking, or swimming, and listen to your body. Gut Health: The foundation of menopause symptom relief When it comes to managing perimenopausal symptoms, whether it’s hot flushes, burning feet, mood swings or sleep disruption, your gut health should be the first place you start when looking to manage your symptoms. Think of it as the foundation of your menopause toolkit. Whether you’re taking HRT or not, a healthy gut sets the stage for better hormonal balance, stronger immunity, and a calmer nervous system[4]. It also helps to: 1. Regulate oestrogen levels naturally Certain gut bacteria, often referred to as the estrobolome, help break down and recycle oestrogen in the body. A balanced gut microbiome means fewer hormonal highs and lows, which can reduce hot flushes, mood dips, and more[5]. 2. Reduce systemic inflammation Chronic inflammation, often driven by gut imbalances, can heighten symptoms like burning skin, joint pain, or general heat sensitivity[6]. By supporting your gut, you’re helping your entire system stay calmer and more resilient. 3. Improve sleep, mood & stress response The gut-brain axis directly affects how well you sleep, how stressed you feel, and how your nervous system responds to temperature and discomfort. A healthy gut helps modulate cortisol (stress hormone) and supports production of mood-stabilising serotonin[7] Feed your gut (with targeted support for women in perimenopause) Gut health is foundational, but not all probiotics are created equal. If you're in your 40s or 50s and navigating perimenopause, supporting your gut with targeted probiotic strains is one of the most effective steps you can take. Why a targeted probiotic like Better Gut matters: Aids in oestrogen metabolism for fewer hormonal spikes Reduces bloating and gut sensitivity often triggered by stress and food changes Supports immune balance, which is crucial as hormone levels shift Helps calm burning sensations and flushes from the inside out Pair with a fibre-rich, gut-loving diet: Eat prebiotic foods like leeks, asparagus, bananas, and oats Include fermented foods (as tolerated) such as kefir or sauerkraut Stay hydrated with water, herbal teas, and mineral-rich broths Final thoughts: Thriving, not just surviving Perimenopause is a natural phase of life, not a medical condition, but that doesn’t mean you have to suffer through it. Whether it’s blazing hot outside or your internal thermostat is having a moment, you can take back control with simple, science-backed strategies. Start with your gut. Support it daily with targeted probiotics and nourishing foods. Hydrate. Cool down. And most importantly, listen to your body with compassion. You’re not just powering through—you’re creating a foundation for the next vibrant chapter of life. References NHS. Menopause symptoms British Menopause Society. Guidance on menopausal symptoms Women's Health Concern. Menopause Fact Sheet National Institutes of Health (NIH). Gut microbiota and menopause: A review Plottel, CS et al. "The human microbiome and estrogen metabolism." Cell Press, Trends in Endocrinology & Metabolism. Cani, PD. "Gut microbiota and inflammation." Current Opinion in Clinical Nutrition, 2011. Mayer, EA. "Gut/brain axis and the microbiota." Journal of Clinical Investigation, 2015. EFSA (European Food Safety Authority). Hydration guidelines NIH. Magnesium: Fact Sheet for Health Professionals. NIH Magnesium National Center for Complementary and Integrative Health. Herbs and Supplements Sleep Foundation. Menopause and Sleep
Read moreBerberine and menopause: A natural ally for weight management
A Natural Way to Support a Healthy Metabolism There’s growing interest in new approaches to weight management, especially those focused on metabolic health and appetite regulation. While some prescription options have made headlines, they often come with side effects and may not offer lasting support once use is discontinued. For those looking for a more natural approach, there’s Berberine, a powerful botanical compound with a long history of traditional use and growing scientific interest. It’s the hero ingredient in our new formula, Better Metabolism. Berberine has been studied for its potential to: Support healthy blood sugar levels already in the normal range Promote energy production Support metabolic function, particularly during midlife These benefits make it a compelling option for those navigating the changes that come with perimenopause and beyond. If you're looking for a gentle, sustainable way to support your metabolism—without harsh stimulants or prescriptions—Berberine could be a valuable tool in your wellness routine. Berberine: Nature’s metabolism ally Berberine has been used for thousands of years in traditional Chinese and Ayurvedic medicine, and modern science now supports its impressive range of benefits. It’s been shown to: Improve insulin sensitivity[2] Lower fasting blood glucose and HbA1c levels[3] Regulate lipid metabolism and reduce triglycerides[4] Activate AMP-activated protein kinase (AMPK) – your body’s metabolic switch[5] Support weight management in insulin-resistant individuals[6] AMPK is the same enzyme activated by exercise and fasting. It tells your cells to shift from “store fat” mode into “burn energy” mode, helping support healthy glucose levels, fat metabolism, and even mitochondrial function. Why we created Better Metabolism At The Better Menopause, we know that midlife metabolic shifts aren’t just about weight, they’re about energy, blood sugar, gut health, and inflammation. That’s why Better Metabolism has been formulated with a blend of complementary high-strength ingredients, including: Berberine – Supports glucose control and AMPK activation Cinnamon extract – Enhances insulin signalling and reduces post-meal blood sugar spikes[7] Chromium – Aids in glucose transport and helps curb sugar cravings[8] Myo-Inositol – Enhances insulin function and supports hormone balance, particularly in PCOS[11 What about your gut health? Berberine doesn’t just support metabolism, it may also play a key role in gut health. Thanks to its natural antimicrobial properties and it’s been used in functional medicine for gut imbalances like SIBO (small intestinal bacterial overgrowth). Early research shows Berberine may actually support the growth of beneficial bacteria, including Akkermansia muciniphila, which is linked to improved metabolic function and gut barrier integrity.[12] To enhance this effect, we recommend pairing Better Metabolism with our targeted gut formula, Better Gut, a targeted probiotic of clinically backed bacterial strains, formulated to rebalance the microbiome and support gut lining integrity during perimenopause and beyond Together, they form a powerful duo for women navigating the metabolic and digestive shifts of midlife. Discover our Body Bundle here Final Thoughts: not a quick fix, a smarter long-term strategy For women in erimenopause and menopause looking to regain balance, Better Metabolism offers a researched, well-rounded solution that supports energy, blood sugar, and fat metabolism, without extreme pharmaceutical intervention for sustained weight management. References Nauck MA, Meier JJ. “Management of endocrine disease: Are all GLP-1 agonists equal in the treatment of Type 2 Diabetes?” Eur J Endocrinol. 2019;181:R211–R234. Chang W, Hatch GM, et al. “Berberine as a therapy for type 2 diabetes and its complications.” Biochem Cell Biol. 2015 Oct;93(5):479-86. Dong H, Wang N, Zhao L, Lu F. “Berberine in the treatment of type 2 diabetes mellitus: a systemic review and meta-analysis.” Evid Based Complement Alternat Med. 2012;2012:591654. Kong W, Wei J, Abidi P, et al. “Berberine is a novel cholesterol-lowering drug working through a unique mechanism.” Nat Med. 2004;10(12):1344-1351. Francini F, Schinella GR, Ríos JL. “Activation of AMPK by Medicinal Plants and Natural Products.” Mini Rev Med Chem. 2019;19(11):880–901. Yin J, Xing H, Ye J. “Efficacy of berberine in patients with type 2 diabetes mellitus.” Metabolism. 2008;57(5):712-717. Cao H, et al. “Anti-diabetic effect of cinnamon: implications for its use in prevention and treatment of Type 2 Diabetes.” Nutr Res Pract. 2007. Anderson RA. “Chromium, glucose intolerance and diabetes.” J Am Coll Nutr. 1998;17(6):548-555. Packer L, Witt EH, Tritschler HJ. “Alpha-lipoic acid as a biological antioxidant.” Free Radic Biol Med. 1995;19(2):227-250. Malaguarnera M. “Carnitine derivatives: clinical usefulness.” Curr Opin Gastroenterol. 2012 Mar;28(2):166–76. Nestler JE, Jakubowicz DJ, et al. “Effects of inositol on ovarian function in women with PCOS.” N Engl J Med. 1999. Dong C, Yu J, Yang Y, et al. “Berberine, a potential prebiotic to indirectly promote Akkermansia growth through stimulating gut mucin secretion.” Biomedicine & Pharmacotherapy. 2021;139:111595.
Read moreCortisol, gut health & menopause: What you need to know
Menopause is a natural transition—but let’s be honest, it doesn’t always feel natural. If you're experiencing fatigue, mood swings, weight gain, brain fog, or sleep issues, you’re not alone. While hormone changes often take the blame, there’s another overlooked culprit: cortisol, your body’s primary stress hormone. What many women don’t realise is how closely cortisol is connected to gut health. This connection influences everything from your mood to your metabolism—and is the reason why many women are turning to targeted gut-supporting supplements like Better Gut to naturally reduce stress and ease menopause symptoms. What is cortisol—and why it matters during menopause Cortisol is produced by your adrenal glands in response to stress. It’s essential for regulating: Your sleep–wake cycle Blood sugar and metabolism Inflammation and immune response Fat storage and energy use However, during menopause, reduced levels of oestrogen and progesterone can make the body more sensitive to cortisol—leading to stronger and longer-lasting stress responses. [1] How high cortisol levels worsen menopause symptoms Hot flushes & night Sweats Cortisol interferes with your hypothalamus, the part of the brain that regulates temperature. This may contribute to the sudden heat surges and night sweats many women experience in menopause. [2] Insomnia & sleep disruption At night, cortisol should naturally drop. But under stress, it can remain elevated—making it difficult to fall asleep or leading to 2–3 a.m. wake-ups. Supporting your nervous system with calming nutrients like ashwagandha, magnesium and vitamin B6—as found in Better Night—can help restore your natural sleep cycle. [3] Mood Swings, anxiety & brain Fog Elevated cortisol can disrupt neurotransmitters in your brain, making it harder to regulate mood and memory. Ingredients like affron® saffron, ashwagandha, and GABA-supportive B vitamins have been shown to ease stress and support mood stability—making targeted support like Better Night a smart addition to your routine. [4] Weight Gain, especially around the middle Cortisol tells your body to store belly fat and triggers cravings for high-sugar, high-fat foods. A healthy gut can help balance these cravings by improving blood sugar regulation and nutrient absorption. [5] Bloating, food sensitivities & inflammation Cortisol compromises your gut lining and microbiome diversity, contributing to systemic inflammation. A high-quality probiotic—like Better Gut—can help repair this balance, supporting digestion and reducing inflammatory symptoms. [6] The gut–cortisol–menopause feedback loop Stress raises cortisol, which damages the gut, leading to inflammation and worsened hormone symptoms—creating a loop that’s hard to break. But research shows that targeting the gut–hormone–stress axis can reduce symptoms holistically. Stress → High Cortisol → Gut Imbalance → More Inflammation → More Symptoms → More Stress This is exactly why many women start by improving their gut health when looking for long-term menopause relief. The role of gut health during menopause There’s a profound connection between your gut and your hormones during menopause. Flutuating hormones disrupt the delicate balance of the gut microbiome leading to a range of symptoms—including bloating, mood swings, brain fog and hot flushes—supporting your gut during this time woth tailored probiotic can help reduce your symtoms as well as helping regulate cortisol, balance oestrogen, and reduce inflammation. Better Gut is a high-strength probiotic supplement formulated with 50 billion CFUs and six targeted bacterial strains selected to support gut and hormone health during perimenopause and menopause. Each strain was chosen for its specific benefits in relieving common menopause symptoms: Lactobacillus rhamnosus – Can help improve stress resilience, reduce anxiety, and ease bloating, inflammation, and vaginal dryness HOWARU® Lactobacillus rhamnosus – A clinically studied strain shown to reduce stress and support emotional wellbeing Lactobacillus acidophilus – Helps protect against vaginal and urinary tract infections by maintaining a healthy vaginal microbiome Bifidobacterium lactis – May help reduce the severity and frequency of hot flushes and night sweats Lactobacillus reuteri – Supports mood balance and sleep quality Bifidobacterium bifidum – Promotes healthy digestion and regularity, helping to relieve menopause-related constipation This targeted blend works in harmony with your body to help restore balance from within—supporting digestion, stress regulation and hormonal health during every stage of menopause. Shop Better Gut and use code WELCOME15 for 15% off your first order. Evening support: How Better Night helps to regulate cortisol Quite often high cortisol levels result in middle of the night wake-up, that's where a adaptogens like Ashwagandha can really support you. Better Night is a non-sedating, hormone-friendly formula designed to support natural sleep cycles disrupted by cortisol. It combines: KSM-66® Ashwagandha – Clinically shown to reduce cortisol and improve sleep quality Affron® Saffron – Improves mood and emotional regulation at night Magnesium Glycinate – A highly absorbable form for calming nerves and muscles Chamomile & Vitamin B6 – To relax the body and support melatonin production These ingredients are ideal for supporting deep, restorative sleep—without next-day grogginess. Try Better Night to wind down, stay asleep, and support your emotional health overnight. Additional lifestyle strategies to naturally lower cortisol In addition to targeted supplements like Better Gut and Better Night, daily habits play a big role in regulating cortisol levels. Here are simple, sustainable strategies that can help support your stress response: Practice daily mindfulness – Just 10 minutes of deep breathing, meditation, or yoga can lower cortisol and improve mental clarity. Prioritise gentle movement – Swap intense workouts for walks, Pilates or tai chi. Overtraining can actually raise cortisol. Eat regular, balanced meals – Skipping meals or restricting carbs can spike cortisol. Include whole grains, lean protein, and healthy fats at each meal. Cut back on caffeine and alcohol – Both can disrupt sleep and elevate cortisol, especially in the evening. Get sunlight exposure in the morning – Helps regulate your circadian rhythm and promotes healthy cortisol patterns. Set consistent sleep and wake times – A regular sleep routine is one of the most effective ways to support hormone balance and reduce stress reactivity. Journal or reflect before bed – Offloading worries in a notebook can quiet your mind and help you sleep more deeply. These lifestyle changes, when paired with targeted support like Better Gut and Better Night, create a solid foundation for navigating menopause with more energy, better sleep, and fewer stress-driven symptoms. Menopause doesn’t have to feel out of control If you’re feeling out of balance, your gut and stress hormones may be to blame. By restoring your gut health and managing cortisol naturally, you can begin to ease symptoms—from sleep issues to mood swings—without relying solely on short-term fixes. Start by giving your body what it needs to self-regulate. Explore our Better Bundle to support your menopause, naturally. References Menopause and the HPA Axis – Otte et al., 2005 Pathophysiology of Menopausal Hot Flushes – Freedman, 2005 Sleep Loss and Elevated Cortisol – Leproult & Van Cauter, 1997 Stress and Brain Function – Lupien et al., 2009 Stress and Body Shape – Epel et al., 2000 Stress and the Gut–Hormone Connection – Chrousos, 2000
Read moreWhy do random chin hairs appear after 40? The surprising truth
You’re casually checking the mirror when, bam! a rogue chin hair appears out of nowhere. If you’ve noticed random chin hairs popping up after 40, you’re not alone. Many women experience these pesky strays, often wondering, Where did that come from? And why does it feel like steel wire?! This article explores the hormonal causes behind post-40 facial hair, why it happens during perimenopause and menopause, and - most importantly - how to manage it safely and effectively. Why do chin hairs appear after 40? The culprit? Hormonal changes. As women enter perimenopause (late 30s to early 40s) and menopause (typically 45+), their oestrogen levels decline, while testosterone remains stable or even increases proportionally. This shift can lead to: ✔ Thicker, darker facial hairs (hirsutism) ✔ A decrease in collagen and skin elasticity(making hair more noticeable) ✔ Faster-growing coarse hairs on the chin, jawline, and upper lip According to the NHS, menopause-related hormonal shifts can affect everything from hair growth to metabolism, leading to noticeable changes in facial hair. The role of hormones: oestrogen vs. testosterone Before 40: Oestrogen keeps testosterone in check, preventing excess hair growth. After 40: With less oestrogen, testosterone has a greater influence, leading to the emergence of random facial hairs This is why some women never had facial hair in their 20s but suddenly find themselves tweezing chin hairs at 45. Other factors that contribute to chin hair growth Besides hormonal changes, other factors can cause those stubborn chin hairs to sprout: Genetics – If your mum or grandmother had chin hairs, you might, too. Polycystic Ovary Syndrome (PCOS) – A common condition causing excess androgens. Stress & Cortisol – High stress levels can impact hormone balance and increase hair growth. Medications – Some drugs (e.g., steroids, hormone therapies) may trigger facial hair. The British Menopause Society notes that changes in hormone levels during menopause may contribute to increased facial hair growth in women. How to get rid of chin hairs (safely & effectively) If the occasional rogue hair doesn’t bother you, that’s perfectly fine! But if you prefer smoother skin, here are some safe removal options: Quick Fixes: Tweezing – Best for a few stray hairs; results last 2-4 weeks. Dermaplaning – Removes fine peach fuzz + exfoliates skin. Longer-Term Solutions: Waxing or Threading – Lasts 4-6 weeks but may cause irritation. Laser Hair Removal – Reduces growth over time (best for darker hairs). Electrolysis – Permanent hair removal by destroying hair follicles. Can probiotics help reduce chin hair growth? Emerging research suggests that probiotics may play a role in balancing hormones during menopause, which could indirectly help reduce unwanted facial hair Menopause disrupts the gut microbiome, affecting hormone metabolism—particularly oestrogen and androgens (like testosterone). Certain probiotic strains, such as Lactobacillus and Bifidobacterium, have been studied for their ability to: Support hormonal balance– Helping regulate oestrogen metabolism, which may prevent excessive androgens from triggering facial hair growth. Improve insulin sensitivity – Studies show that hormonal imbalances and insulin resistance are linked to excess hair growth (hirsutism) in some women. Probiotics may help stabilise blood sugar, reducing excess androgens Reduce inflammation – A healthy gut can help reduce inflammation-related stress on hair follicles, which may contribute to hair thinning or excess growth. How can probiotics help? If you’re looking for natural ways to support hormonal balance, a high-quality menopause-specific probiotic supplement may be beneficial. Look for clinically studied probiotic strains like those in the Better Gut probiotic. Support with a balanced diet rich in fibre, fermented foods, and hormone-friendly nutrients. While probiotics won’t remove chin hairs overnight, they can support your body’s natural hormone regulation, making them a complementary option alongside other treatments. Want to learn more? Explore our probiotic formula for menopause here. When to See a Doctor If chin hair growth is sudden, excessive, or accompanied by other symptoms (like irregular periods, weight gain, or acne), it may signal an underlying condition like PCOS or adrenal issues. A doctor can check hormone levels and recommend treatments. Final Thoughts Random chin hairs after 40 are a natural part of ageing and hormonal shifts, but they don’t have to be a nuisance. Understanding why they appear and knowing how to manage them can make the process a little less annoying. References: 1. NHS – Menopause and Hormone Changes. (Accessed: March 2024) https://www.nhs.uk/conditions/menopause/ 2. British Menopause Society – Hirsutism in Menopause. (Accessed: March 2024) https://thebms.org.uk/ 3. Probiotics and Hormonal Balance in Menopause: A Review. (2021) [https://pubmed.ncbi.nlm.nih.gov/34109594
Read moreSaffron for Menopause Relief: A Natural Way to Support Mood, Sleep & Libido
For many women in their 40s and 50s, perimenopause and menopause can feel like an emotional and physical upheaval. Mood swings, anxiety, disrupted sleep, low libido, and hot flushes are all too common. While hormone replacement therapy (HRT) and antidepressants are often prescribed, a growing number of women are seeking natural, evidence-based solutions to support their wellbeing during this life stage. One promising option is saffron – not just a culinary spice, but a clinically researched botanical that has shown real benefits for mood, sleep, and emotional balance. A patented extract called Affron® has been the focus of multiple human studies and is featured at the full clinical dose of 30 mg in our supplement, Better Night™ – a natural sleep and stress formula designed specifically for women in midlife. Why Saffron? Saffron (Crocus sativus) contains active compounds like crocin and safranal, which influence key brain chemicals involved in mood regulation – including serotonin, dopamine, and norepinephrine. These neurotransmitters are often impacted during perimenopause and menopause, contributing to anxiety, low mood, and irritability. Saffron works by gently supporting this neurochemical balance, without acting as a hormone. Unlike phytoestrogens or synthetic hormones, saffron does not mimic oestrogen or disrupt endocrine function. This makes it a safe and versatile option, especially for women who cannot or choose not to take HRT. Backed by Clinical Research One of the largest menopause-focused studies on saffron involved 86 women aged 40 to 60 who took 28 mg of Affron® saffron extract daily for 12 weeks. According to the results published in the Journal of Menopausal Medicine, participants experienced: A 33% reduction in anxiety symptoms A 32% reduction in depressive symptoms Significant improvement in emotional wellbeing without any major side effects Read the study summary here. Better Night™ contains 30 mg of Affron® – slightly more than the clinically studied dose – to ensure full support for mood balance, calm, and mental clarity during perimenopause. Sleep Support Without Hormones Insomnia and sleep disturbances are among the most frustrating menopause symptoms. Night sweats, stress, and shifting hormones can make restful sleep elusive. Fortunately, saffron has also been shown to help improve sleep quality in several studies. In a placebo-controlled trial involving adults with poor sleep, both 14 mg and 28 mg of Affron® saffron taken daily improved: Sleep latency (falling asleep faster) Sleep duration Morning energy and alertness View the full study results here. Better Night™ includes 30 mg of Affron® to help you fall asleep more easily, sleep more deeply, and wake up feeling rested. Libido and Intimacy A decline in sexual desire is another common (and often distressing) symptom of menopause. Stress, fatigue, low mood, and hormonal shifts can all dampen libido. Saffron, traditionally used as an aphrodisiac, is now supported by modern science for its role in improving sexual function in women. In a clinical trial, women taking 30 mg of saffron daily for 6 weeks experienced: 62% improvement in their Female Sexual Function Index (FSFI) scores Greater desire, arousal, lubrication, and satisfaction Read the full trial on PubMed. Better Night™ supports libido both indirectly through mood and stress support, and potentially directly through saffron’s role in supporting pleasure-related neurotransmitters like dopamine. What About Hot Flushes? Although saffron is not a direct treatment for hot flushes, it may help by calming the nervous system and reducing the anxiety and stress that often intensify them. Since hot flushes can be triggered by emotional stress or disrupted sleep, saffron’s mood-stabilising and sleep-supporting effects can make them less frequent or easier to manage. Some women who use Better Night™ report that while their flushes haven't disappeared entirely, they feel more resilient and less reactive, thanks to better emotional regulation and more consistent rest. Why Choose Better Night? Better Night is uniquely formulated for women navigating the menopause transition, offering: 30 mg of clinically studied Affron® saffron extract A non-hormonal, non-sedative formula Support for mood, sleep, stress, and libido A trusted, natural solution backed by science Shop Better Night now. The Takeaway Perimenopause and menopause don’t have to mean giving up on restful sleep, emotional balance, or intimacy. Nature provides options – and saffron, especially the clinically tested Affron® extract, is one of the most promising. Better Night™ combines the full clinical dose of Affron® (30 mg) in a simple daily capsule, supporting better sleep, improved mood, and enhanced resilience during the menopause transition – without the use of hormones or harsh medications. Explore Better Night today and discover a natural way to restore calm, clarity, and comfort during midlife. References Lopresti, A. L., & Smith, S. J. (2021). The effects of a saffron extract (Affron®) on menopausal symptoms in women during perimenopause. NutraIngredients. Lopresti, A. L., et al. (2020). Effects of saffron on sleep quality in healthy adults. NeurologyLive. Kashani, L., et al. (2022). Crocus sativus (saffron) in the treatment of female sexual dysfunction. PubMed. Montemarano, M. (2021). Saffron extract may help menopause symptoms. Nutraceuticals World. Psychiatric Times (2019). Is there a role for saffron phytotherapy in treating depression? Psychiatric Times.
Read moreWinter Hormone Health: Top Ten Tips for Supporting Your Well-being
As the New Year begins, it’s the perfect time to focus on your health and set a strong foundation for the months ahead.
Read moreThe Top 10 Nutritional Benefits of a Traditional Christmas Dinner for Women’s Health
A traditional Christmas dinner isn’t just a festive indulgence; it’s a meal brimming with nutrients that can support women’s health, particularly during perimenopause.
Read moreHow menopause affects metabolism and how to improve yours
What is metabolism, how is it affected by menopause and how can you boost yours to improve your health?
Read moreUnderstanding menopause weight gain
Hormone changes, muscle loss and poor sleep can lead to weight gain and increased belly fat during perimenopause and menopause – but there are things you can do to manage it.
Read moreLifestyle tips for losing weight during menopause – and keeping it off
How to support sustainable weight loss during menopause – what to eat, what to limit, the best forms of exercise and tips for better sleep.
Read moreThe links between menopause and leg pain, and the approaches that could help
What does menopause leg pain feel like, what’s the link to changing hormone levels and what could help ease your symptoms?
Read moreImproving your diet for healthy menopause weight loss
Discover the dietary changes you can make to lose menopause weight and belly fat in a sustainable and healthy way, and get inspiration planning your meals.
Read moreNatural supplements that may help with menopause weight loss
We assess the evidence that these natural supplements could aid weight loss and reduce belly fat during menopause, and look at what else you can do to maintain a healthy weight.
Read moreWhat causes menopause brain fog and what can you do about it?
Discover the links between menopause, hormones and brain fog, how long it lasts and the treatments, supplements and lifestyle changes that could help.
Read moreCan your GP prescribe testosterone for menopause?
Learn why testosterone is unlicensed for women in the UK, when it can be prescribed on the NHS, how to get a private prescription and where you can buy testosterone.
Read moreWhy testosterone is important for women and how it could help during menopause
Discover why your body needs testosterone, how testosterone therapy could help during menopause and where you can get it.
Read moreWhat’s causing your burning feet during menopause, and what could help?
Exploring the links between menopause, hormone changes, vitamin deficiencies and hot or burning feet, plus the treatments that could improve your symptoms.
Read moreMedication, supplements and tips to boost your sex drive during menopause
How menopause affects your sex drive and sexual health, and what you can do to increase your libido and make sex more pleasurable.
Read moreHow vitamin D can help with menopause
Everything you need to know about vitamin D and menopause, including the causes and signs of vitamin D deficiency, the best types, how much to take and the symptoms it can help with.
Read moreHRT alternatives and complementary approaches
Learn about the herbal blends, probiotics, lifestyle changes and other prescription drugs that could help with menopause symptoms as an alternative to HRT, or alongside it.
Read moreHow does menopause effect ADHD and could it lead to a diagnosis?
Discover the links between menopause and ADHD, how hormone changes could lead to a diagnosis and what you can do to help relieve your symptoms.
Read moreUnderstanding menopause anxiety and natural ways to manage it
How to spot menopause anxiety, the role fluctuating hormones play, how long it could last, where HRT comes in and some natural ways to manage it.
Read moreMenopause burning mouth, dry mouth, sores and ulcers
Learn about the possible causes of burning mouth syndrome during menopause, the links to other oral health conditions and what can you do to treat your symptoms.
Read moreWhy your body odour could change during menopause, and what you can do about it
Exploring the hormone changes and other factors that can affect body odour during perimenopause and menopause and what you can do to manage it.
Read moreWhat Happens to Your Period During Perimenopause?
Thought you knew exactly where you were with your cycle, until all of a sudden everything changed? Erratic periods, heavy flow, longer cycles, shorter cycles… The possibilities are endless when it comes to perimenopause! So what exactly happens to your period during this time, and what can you do to manage the uncertainty of it all? Award winning GenM (and menopause friendly!) period brand, WUKA, explains more. What is Perimenopause? Most of us learned about the first period at school, but nobody really about the last period, let alone what happens to your cycle in the lead up to that very last bleed. The transition from regular cycles to menopause is called Perimenopause, and thankfully the conversation surrounding it is starting to open up, and we’re starting to understand more about what happens during this time. For some, perimenopause can last up to 10 years, and the age at which it starts can vary form person to person too. What Happens During Perimenopause? During perimenopause the ovaries gradually begin to stop working. It’s a natural process that will happen to us all eventually, and it brings with it quite a range of symptoms, most common of which include: Hot flushes Night sweats Heavy periods Mood swings There are actually a range of other physical and emotional symptoms that can occur too- and changes to your period are, for many, a first sign that perimenopause has begun. Changes to Your Period Fluctuating hormones are at play here. So what can we expect? Shorter Cycles The slowing down of the ovaries can cause the follicular phase to become shorter, which in turn leads to early ovulation- and therefore a shorter cycle overall. Longer Cycles Just like above, longer cycles are also caused by fluctuating hormone levels, and your actual period could last longer than your usual 2-5 days too. Changes to your flow Lots of women going through perimenopause experience changes to their flow, again thanks to fluctuation of hormones. For many, the drop in progesterone can trigger heavy bleeding, and this is very common during the early stages of perimenopause. But just to make it interesting, some cycles may be lighter than usual, and others may be heavier (whilst also being shorter, then longer, then shorter again… ) - so just what is happening here? Hormones, hormones, hormones. As the ovaries slow down, they might not produce an egg for ovulation during some cycles. This is called an anovulatory cycle, and results in a lighter blood flow. When ovulation does occur, your period will be heavier- and if your cycle has been longer than normal, your flow could be heavier than normal too. Towards the end of perimenopause, fluctuations of hormones become a little more intense, and variations in your cycle can occur more and more. In other words, you might not know what’s happening or when! Managing Your Period During Perimenopause It’s not easy trying to predict how your cycle is going to behave from one month to the next, and if you’ve always been regular it can be quite frustrating too. So how do we manage our period with all of this uncertainty? Make the switch to period pants. Here are just three reasons why it’s a good idea: Leak-free confidence: When your flow is super heavy, the last thing you want is to spend half the day in the loo changing leaking pads or tampons. WUKA’s Super Heavy Flow period pants hold up to 60ml period blood, meaning you can wear them for longer without fear of leaks. Yes, even at nighttime. Thanks to an extra long gusset, these pants are guaranteed to hold it all in, all while keeping you feeling fresh and dry too. Just-in-case-reassurance: Erratic cycles can be hard to navigate, and nobody has the spare cash to waste on plastic-filled disposables that might or might not be needed. Luckily, period pants can be worn just like normal underwear, ready to absorb your flow if it decides to turn up. And if it doesn’t, just wash them with your normal laundry load and they’re ready to go for next time. Stay cool, stay comfy: Cycle changes aren’t the only symptom of perimenopause- temperature fluctuations, bloating, weight gain, cramps and vaginal dryness are all symptoms that could pop up as part of this journey towards menopause. And that’s on top of an erratic period! Don’t worry, WUKA period pants have got it covered. Their Stretch™ period pants feature CoolMax™ technology to keep you dry and fresh, and Stretch™ technology for a second-skin fit. This means that even if your flow is heavy, the blood will stay locked away from your body and you’ll stay comfy and odour-free. It also means that you’re guaranteed a perfect fit (each pair stretches up to 4 sizes) even if you’re bloated or you've gained some weight. No digging in and no chafing whatsoever- plus the Cotton Stretch™ period pants offer protection against irritation too. How to use period pants It’s never too late to make the switch to period pants, and they’re so easy to use. Wear like normal underwear, bleed into them, wash them. That’s it! After use, rinse in cold water as soon as you can, then wash as normal on a low heat setting (no hotter than 40 degrees), then either dry outdoors or inside on an airer. No fabric conditioner or tumble dryers. You’ll need around 5 pairs of pants per cycle- that’s one pair to wear, one pair for spare and one pair for nighttime, with two in the wash/ for extra heavy flow days. They’ll last up to two years if cared for properly, and can be used to absorb all the way from light flow (including spotting and/ or discharge) to super heavy flow. We also recommend WUKA DryTech™ reusable incontinence pants for lights leaks and dribbles (yet another delight of perimenopause- 1 in 3 women experience bladder weakness over the age of 35!). These pants also use their innovative Stretch™ technology so adjust up to 4 sizes in one pair. If you would like to try WUKA pants for your then head on over by clicking here and use code BETTERM10 for 10% off your first purchase.
Read moreWhat is restless legs syndrome and how is it linked to menopause?
Exploring the connection between restless legs syndrome and menopause, what it feels like and what you can do to relieve it.
Read moreMenopause mood changes and what you can do about them
Discover the links between menopause, perimenopause and mood symptoms, as well as the lifestyle changes, supplements and other treatments that could help.
Read moreHow menopause affects your sleep, and how you can improve it
Exploring the links between menopause, perimenopause and sleep problems, plus the natural remedies, treatments and supplements that could help.
Read moreNavigating HRT – Everything you need to know
Navigating HRT – Everything you need to know By Dr Rachel Hines Hormone replacement therapy (HRT) plays a vital role in managing menopause symptoms for many people, but it’s not for everyone. Some rave that it changed their life, others try it for six months but don’t get on with it. Some people never need or just don’t want it. Whether you're actively seeking help for your symptoms or just want to learn more about menopause, understanding how HRT works and who it can help is key. Here, we explore its benefits, when to consider it and treatment alternatives if it’s not for you. What is HRT? As the name suggests, hormone replacement therapy (HRT) is a kind of medication that supplies your body with hormones that are produced at lower levels during menopause. It has been consistently proven to be the most effective treatment for a range of menopause symptoms such as mood changes, hot flushes, painful sex and bladder symptoms. What are the different types of HRT? There are three different hormones you may need during menopause and two main types. Each hormone can also be taken in different ways, such as transdermally (through the skin) through a patch, cream or gel, or orally, as a tablet. Your doctor will help you decide which hormones and products are right for you. Here’s a summary of some of the options you may discuss. Oestrogen Menopause symptoms are mainly caused by fluctuating and declining oestrogen levels. Supplying your body with this hormone helps improve many menopause symptoms, which may include hot flashes, mood swings, vaginal dryness or trouble sleeping. Read more about the 34 symptoms of menopause. Progesterone Progesterone is prescribed alongside oestrogen if you still have your womb. When used alone, oestrogen can cause the lining of the womb to thicken, which increases the risk of developing womb cancer Thankfully, using progesterone alongside oestrogen removes this risk. Taking oestrogen and progesterone together is called combined HRT. Testosterone Testosterone is relatively new to the HRT scene. It is currently only prescribed for people who are stable on their systemic HRT (oestrogen with or without progesterone) and are still experiencing low libido. Read more about testosterone HRT. Systemic HRT This is HRT that is absorbed into the bloodstream and has effects across your body. This means it is used to treat body-wide - also known as systemic - menopause symptoms. Oestrogen, progesterone and testosterone can all be taken systemically. Vaginal oestrogen Vaginal HRT is applied inside your vagina - or to the wider genital area - and only works in the area where it is applied. It is a great option for people with vaginal, vulval or urinary symptoms, and can be used either alone or alongside systemic HRT. Vaginal HRT is always oestrogen only. Unlike other forms of oestrogen, you do not need to use progesterone if you’re taking vaginal oestrogen alone.There are quite a few more complexities to explore, but that covers the basics! When should you start HRT? There is no single answer to this question - we are all very different. Ultimately, it is your choice, and your doctor can help you make an informed decision once they are sure that menopause is behind your symptoms. Questions to consider together include: Are you open to hormonal treatment? Is HRT a safe option for you? How are your menopause symptoms impacting your life? And what does science say? It's best to start HRT within ten years of menopause and before the age of 60 to gain maximum cardiovascular benefits, according to research. Cardiovascular health relates to the health of the heart and blood vessels. Your doctor will usually advise you to start HRT straight away if you are diagnosed with premature ovarian insufficiency. Read more about when to start HRT. What are the risks and benefits of HRT? These will be different for everyone, as we all have a unique menopause experience and individual risk factors linked to our personal or family medical histories. The risks and benefits are also unique to the type of HRT you take. Benefits of HRT Menopause symptom relief is the main benefit of HRT. It is the most effective treatment for many menopause symptoms, including: Night sweats Hot flushes Mood changes, including low mood Sleep issues Genitourinary syndrome of menopause - this is an umbrella term for vaginal and urinary symptoms such as vaginal dryness, painful sex and frequent urination There are some other benefits too. HRT may also help: Protect the health of your bones, according to research Protect your heart and blood vessels- research suggests this happens if you start HRT within 10 years of menopause or before the age of 60 Reduce your risk of bowel cancer, as emerging evidence suggests Risks of HRT As with any medication, there are also risks to consider. These risks do not apply to all types of HRT and will be more or less important depending on your medical history. Increased risk of breast cancer. Oestrogen-only HRT - including vaginal HRT - causes little or no change to your risk of breast cancer. Combined HRT (oestrogen and progesterone) may increase your risk - about as much as drinking two or more units of alcohol per day, and not as much as being overweight. Increased risk of blood clots with oral HRT (tablets) Increased risk of stroke with oral HRT (tablets), more so when started in women over the age of 60 It is worth reading more about the benefits and risks of HRT to help inform your decision. There is still a lot for scientists to discover, but we know more now than ever before. Who can take HRT? You will be prescribed HRT if the benefits outweigh the risks for you personally. Due to the risks outlined above, doctors will not generally prescribe systemic HRT if you have any of the following: Breast cancer, whether past, present or suspected Known or suspected oestrogen-dependent cancers (meaning those which grow in response to oestrogen, most often in the breast, ovary, womb or endometrium) Certain types of arterial disease such as angina or heart attack Unexplained vaginal bleeding Untreated endometrial hyperplasia (abnormal thickening of the lining of the womb) Certain types of venous thromboembolism (blood clots) including pulmonary embolism (PE) and deep vein thrombosis (DVT), unless you are already on medications to thin the blood (anticoagulants) Thrombophilic disorders (conditions which increase your blood’s tendency to clot) Liver disease with abnormal blood tests Pregnancy Systemic HRT can sometimes be used for women with the above risk factors under specialist guidance. You may also still be able to take vaginal HRT even if you are not eligible for systemic treatment. There are a few other conditions and risk factors that may influence your doctor when prescribing HRT. Fortunately, there are other ways to treat and manage your menopause symptoms if HRT is not a safe recommendation for you. What can you do if you can't take HRT? Both non-hormonal medications and lifestyle changes can help manage common symptoms. Many people combine these approaches - sometimes it takes a bit of trial and error to find your most effective solution. Hot flushes Non-hormonal medications that can help hot flushes and other menopausal symptoms include: SSRI antidepressants, such as sertraline, citalopram or fluoxetine Clonidine Gabapentin Fezolinetant (Veozah) - a new medication now available in the UK on private prescription. Bladder and vaginal issues Vaginal oestrogen is the most effective treatment for the genitourinary syndrome of menopause (GSM), which includes symptoms like increased urinary frequency, vaginal dryness and painful sex. Itis generally safe to use, even if combined HRT is too risky for you. Non-hormonal options include: Vaginal moisturisers. These are widely available to help vaginal dryness or painful sex Lubricants. Try a pH-balanced lubricant to relieve painful sex Other symptoms Many lifestyle changes can have a huge impact on your menopause symptoms, including hot flashes, sleep issues, anxiety, bladder and vaginla symptoms and low mood. Try to: Get enough exercise Maintain a healthy weight Eat a nutritious diet Consider decreasing your caffeine, alcohol and/or nicotine intake Summary HRT may not be suitable for you because of your medical history or you may just prefer not to take it. That’s ok, HRT isn’t for everyone - there are alternative, non-hormonal medications and lifestyle change can make a real difference too. Your doctor will help you make an informed decision. If you would like to find out what your treatment options are, we have partnered with online menopause clinic, Stella, to give you access to their tailored menopause care. With Stella, you can skip NHS waiting times and talk to a doctor who has additional training in women’s health within a week. They will explain your options and if HRT is suitable, then send it to you in the post. You also get access to the Stella menopause app, where you can follow self-guided lifestyle change plans, speak to a real-life coach and try menopause-friendly workouts and recipes. All this for just £135. Take Stella’s assesment today. About the author Dr Rachel Hines Clinical Director of Menopause Services at Stella Dr Rachel is a GP and expert in menopause health. She has completed advanced menopause training with the Faculty of Sexual and Reproductive Healthcare and is on the British Menopause Society specialist register. She also has diplomas in sexual and reproductive healthcare, gynaecology and child health, and has specialised in women’s health throughout her career.
Read moreWhat causes menopause fatigue and what can you do about it?
From low energy to crashing fatigue, menopausal hormone changes could be causing your tiredness. Discover how the two are linked and what you can do to improve things.
Read more10 ways to tackle your menopause anxiety
We assess herbal remedies, supplements, lifestyle changes and other treatments that may help with anxiety during perimenopause and menopause.
Read moreNatural remedies for menopause mood swings and low mood
Experiencing irritability, mood swings or low mood? These herbal remedies, probiotic supplements, mindfulness approaches and lifestyle tips could help.
Read moreDoes menopause cause constipation, and what can you do?
Discover the connections between fluctuating hormones and constipation, plus the natural remedies, lifestyle changes and treatments that can help.
Read more